Upper GI bleeding means blood loss from the food pipe (esophagus), stomach, or duodenum. It shows up as vomiting blood, passing black tarry stool, or both — and it is always a reason to see a doctor the same day. This page covers every warning sign, the six major causes, how doctors confirm the diagnosis, and the treatment pathway used in Vadodara.
Quick Answer
What Is Upper GI Bleeding?
Upper gastrointestinal bleeding is one of the most common reasons for emergency hospital admission worldwide — and in India, it remains a leading cause of preventable death when patients present late. The numbers are straightforward: early endoscopy within 24 hours reduces re-bleeding, the need for surgery, and mortality. Delay does the opposite.
This page is the comprehensive disease-and-warning guide. If you came here after noticing black stool alone, that companion page covers the symptom-level triage (iron tablets vs real bleeding). This page goes further — it covers the full clinical picture including hematemesis, all six major causes, clinical scoring, the diagnostic pathway, and every treatment step from resuscitation to surgery.
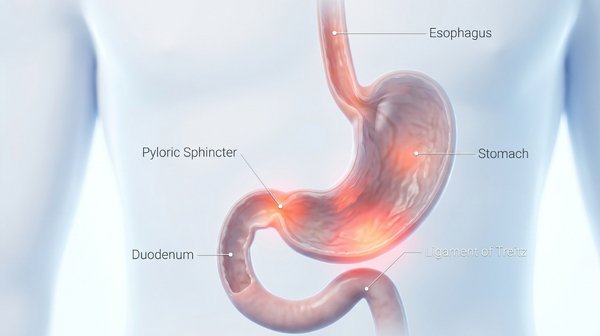
The gastrointestinal tract is divided into upper and lower segments by a small fold of tissue called the ligament of Treitz, located where the duodenum meets the jejunum. Any bleeding that originates above this point is classified as upper GI bleeding (UGIB). The upper tract includes three structures: the esophagus (food pipe), the stomach, and the duodenum (the first part of the small intestine).
Upper GI bleeding accounts for roughly 80% of all acute GI bleeds seen in emergency departments. It can range from a slow ooze that causes anaemia over weeks to a massive arterial bleed that drops blood pressure within minutes. The presentation depends on two things: the speed of bleeding and the volume of blood lost.
Melena vs Hematemesis: The Two Faces of Upper GI Bleeding
Upper GI bleeding announces itself through two distinct symptoms. Understanding the difference matters because it tells the doctor something about where and how fast the bleeding is occurring.
Hematemesis vs Melena — Key Differences
Hematemesis (Vomiting Blood)
- Vomiting fresh red blood — suggests active, brisk bleeding
- Vomiting dark "coffee-ground" material — blood that sat in the stomach and was partly digested by acid
- Often from stomach ulcers, varices, or Mallory-Weiss tears
- Usually prompts patients to seek help immediately
- Volume can range from streaks to large clots
Melena (Black Tarry Stool)
- Jet black, sticky, shiny stool with a strong foul smell
- Blood has been chemically changed by stomach acid during transit
- Needs only 50-100 ml of blood to appear
- Can persist for 3-5 days after a single bleed
- Often underestimated by patients — many wait days before seeking help
- Not the same as dark stool from iron tablets or food
Some patients have both hematemesis and melena simultaneously. A small number with very rapid upper GI bleeding may pass fresh red blood per rectum (hematochezia) — which can initially mislead clinicians into thinking the source is in the colon. This is why endoscopy of the upper tract is done first in any patient with significant bleeding and haemodynamic instability.
Causes of Upper GI Bleeding
Six conditions account for the vast majority of upper GI bleeds. The table below summarises each, followed by a detailed explanation.
| Cause | Approximate share | Key risk factors |
|---|---|---|
| Peptic ulcer (gastric or duodenal) | 40-50% | NSAIDs, H. pylori, smoking, alcohol |
| Erosive gastritis / gastropathy | 15-20% | NSAIDs, alcohol binges, critical illness |
| Esophageal or gastric varices | 10-15% | Cirrhosis, portal hypertension, alcohol-related liver disease |
| Mallory-Weiss tear | 5-10% | Forceful vomiting, retching, alcohol |
| Esophagitis / reflux ulcers | 5-10% | Long-standing GERD, obesity, hiatal hernia |
| Upper GI cancer (stomach or esophagus) | 2-5% | Age >55, weight loss, dysphagia, family history |
1. Peptic Ulcer Disease
A crater in the stomach lining (gastric ulcer) or in the duodenum (duodenal ulcer) that erodes into a blood vessel. This is the single most common cause of upper GI bleeding worldwide. Two forces drive peptic ulcer: infection with the bacterium Helicobacter pylori and chronic use of NSAIDs (diclofenac, ibuprofen, aspirin, naproxen). When both are present, risk multiplies. Patients typically describe a burning or gnawing pain in the upper abdomen that worsens on an empty stomach. Many have taken painkillers for months before the bleed occurs.
2. Erosive Gastritis
Widespread shallow inflammation of the stomach lining rather than a single deep ulcer. Common triggers include heavy alcohol intake, daily NSAID use, severe physiological stress (ICU admission, major trauma, extensive surgery), and bile reflux. Bleeding is usually less dramatic than ulcer bleeding but can cause persistent melena and significant anaemia over days.
3. Esophageal and Gastric Varices
In patients with cirrhosis or other causes of portal hypertension, the veins in the lower esophagus and upper stomach become swollen and fragile. When a varix ruptures, the bleeding is often sudden, massive, and life-threatening. Patients may vomit large volumes of fresh blood and go into shock within minutes. Variceal bleeding carries the highest mortality of all upper GI bleed causes and requires emergency endoscopic band ligation.
4. Mallory-Weiss Tear
A longitudinal tear at the junction between the esophagus and stomach, caused by forceful or prolonged vomiting. The classic history is a patient who vomited several times (often after alcohol or during a viral illness), then noticed blood in the vomit. Most Mallory-Weiss tears heal on their own within 48-72 hours, but a deep tear can bleed briskly and require endoscopic clipping.
5. Esophagitis and Reflux Ulcers
Chronic acid reflux erodes the lower esophagus over months to years. The bleeding is usually slow and presents as iron-deficiency anaemia and occasional dark stool rather than dramatic hematemesis. However, a deep reflux ulcer can cause a significant acute bleed. Patients with untreated acid reflux for years are at highest risk. Treatment involves acid suppression and, when appropriate, anti-reflux surgery — see our GERD surgery page.
6. Upper GI Cancer
Stomach cancer and esophageal cancer can both present with upper GI bleeding. The bleed is often chronic and low-grade — patients notice fatigue, pallor, and weight loss before they notice blood. Warning signs that raise suspicion for cancer include unexplained weight loss, difficulty swallowing, early fullness after small meals, persistent vomiting, and age over 55 with new-onset symptoms. Early endoscopy is the only reliable way to rule it out.
Red Flag Warning Signs — Seek Emergency Care
- Vomiting fresh red blood or large volumes of coffee-ground material
- Black, tarry, sticky, foul-smelling stool (melena)
- Dizziness, light-headedness, or fainting — especially on standing
- Rapid heartbeat (>100/min) at rest with cold, clammy skin
- Pale skin, pale nail beds, pale conjunctiva
- Confusion or drowsiness in an otherwise alert person
- Known history of liver cirrhosis, varices, or previous GI bleed
- Currently taking blood thinners (warfarin, heparin, DOACs)
- Weight loss + difficulty swallowing with any bleeding sign
If any of these apply, go to a hospital emergency department now. Upper GI bleeding can deteriorate rapidly — hours matter.
How Doctors Assess Severity: Glasgow-Blatchford and Rockall Scores
When a patient arrives in the emergency department with suspected upper GI bleeding, the clinical team uses validated scoring systems to decide how urgently endoscopy is needed and whether the patient requires ICU admission.
Glasgow-Blatchford Score (GBS)
This is the most widely used pre-endoscopy scoring tool. It uses simple parameters available at the bedside: haemoglobin level, blood urea, systolic blood pressure, pulse rate, presentation with melena or hematemesis, presence of syncope, and history of liver or heart disease. A score of 0 identifies very-low-risk patients who may be safely managed as outpatients. A score of 6 or above indicates a high likelihood of needing intervention (transfusion, endoscopic therapy, or surgery).
Rockall Score
The Rockall score has two versions. The pre-endoscopy (clinical) Rockall uses age, shock status, and comorbidities. The full Rockall score adds endoscopic findings — the specific diagnosis and the presence of stigmata of recent haemorrhage (visible vessel, adherent clot, active spurting). It is primarily used to predict re-bleeding risk and mortality after endoscopy.
In practice, most emergency departments in India use the Glasgow-Blatchford score to triage patients. A high score means early endoscopy (within 12-24 hours), aggressive resuscitation, and close monitoring.
Diagnosis: How the Bleeding Source Is Found
The diagnostic pathway for upper GI bleeding is focused and time-sensitive. In Vadodara, the standard approach at Sterling Hospital follows international guidelines.
1. Clinical Assessment and Resuscitation
The first priority is always haemodynamic stability. Two large-bore IV lines, rapid fluid infusion, and blood sent for haemoglobin, coagulation profile, kidney function, liver function, and cross-match. A thorough history covers NSAID use, alcohol, liver disease, previous bleeds, anticoagulants, and recent vomiting. Examination checks pulse, blood pressure (lying and standing), pallor, signs of chronic liver disease (jaundice, ascites, spider naevi), and abdominal tenderness.
2. Upper GI Endoscopy — The Primary Investigation
Upper GI endoscopy (also called OGD or gastroscopy) is the
single most important test. A thin flexible camera is passed through the mouth under short
sedation to directly inspect the esophagus, stomach, and duodenum. It identifies the bleeding
source in approximately 90% of patients. Critically, it allows treatment during the same
procedure — injecting adrenaline into a bleeding ulcer, applying thermal coagulation, placing
haemostatic clips, or banding a variceal vessel.
International guidelines recommend endoscopy
within 24 hours for all patients with upper GI bleeding, and within 12 hours for high-risk
patients (those with haemodynamic instability, active hematemesis, or a Glasgow-Blatchford score
above 12).
3. Blood Tests
Haemoglobin measures blood loss severity (though it may be falsely normal in the first 6-8 hours of acute bleeding as haemodilution has not yet occurred). Blood urea is often elevated in upper GI bleeding because digested blood acts as a protein load. Coagulation studies and platelet count are essential, especially in patients on anticoagulants or with liver disease.
4. Additional Investigations
If endoscopy does not identify the source (about 10% of cases), further options include CT angiography, tagged red-cell nuclear scan, capsule endoscopy, or angiographic embolisation. A colonoscopy may be added to rule out a lower GI source when the presentation is ambiguous.
Treatment: Stabilise, Scope, Treat, Prevent
The treatment of upper GI bleeding follows a four-step framework used in every major hospital: stabilise the patient, find the source with endoscopy, treat the source, and then prevent recurrence.
Step 1: Immediate Stabilisation
- Intravenous crystalloid fluids to restore circulating volume
- Blood transfusion — indicated when haemoglobin drops below 7 g/dL, or earlier if the patient is haemodynamically unstable or has cardiac disease
- Intravenous proton pump inhibitor (PPI) bolus followed by infusion — this raises gastric pH, stabilises clots on ulcers, and reduces the risk of re-bleeding before endoscopy
- Correction of coagulopathy — vitamin K, fresh frozen plasma, or platelet transfusion as needed
- For suspected variceal bleeding: intravenous terlipressin or octreotide to reduce portal pressure while awaiting endoscopy
- ICU or high-dependency admission for unstable patients
Step 2: Endoscopic Treatment
- Peptic ulcers: injection of dilute adrenaline + thermal coagulation or haemostatic clips. Combination therapy is more effective than any single method.
- Varices: endoscopic band ligation is the standard. Sclerotherapy is an alternative when banding is technically difficult.
- Mallory-Weiss tears: most stop spontaneously. Active bleeders are treated with clips or injection.
- Dieulafoy lesions: clip application or thermal coagulation.
- Tumour bleeding: temporary haemostasis with injection or coagulation while planning definitive surgery or oncology referral.
Step 3: Medical Therapy After Endoscopy
- H. pylori eradication: 14-day triple or quadruple therapy in all H. pylori-positive ulcer patients. Confirmation of eradication 4 weeks later with a breath or stool test.
- PPI maintenance: continued oral PPIs for 4-8 weeks to allow ulcer healing, and long-term in patients who must remain on anticoagulants or low-dose aspirin.
- NSAID review: stop the offending drug if possible. If pain relief is essential, switch to paracetamol or a COX-2 selective agent with a PPI cover.
- Variceal prophylaxis: non-selective beta-blockers (propranolol or carvedilol) plus repeat banding sessions until varices are obliterated.
- Iron replacement: for patients discharged with anaemia.
Step 4: Surgery
Surgery is reserved for the small percentage of patients in whom endoscopy fails to control bleeding (typically after two endoscopic attempts), those with a perforation alongside bleeding, and patients with a bleeding upper GI cancer requiring resection. Laparoscopic approaches are used wherever feasible — smaller incisions, shorter hospital stays, and faster return to normal activity.
What Happens If Warning Signs Are Ignored?
Upper GI bleeding has a built-in pattern that punishes delay. Patients who present within 24 hours generally do well. Those who wait — hoping the symptoms will resolve with home remedies, antacids, or rest — face progressively worse outcomes.
- Severe anaemia and organ damage. A bleeding ulcer can drop haemoglobin from a normal 14 g/dL to 5-6 g/dL over a week. At that level, the heart, kidneys, and brain are all at risk. Elderly patients are especially vulnerable to heart attacks triggered by anaemia.
- Haemorrhagic shock. A sudden large bleed — from a posterior duodenal ulcer eroding into the gastroduodenal artery, or from a ruptured varix — can cause life-threatening shock within an hour. Without immediate resuscitation, mortality is high.
- Re-bleeding. An untreated ulcer that has bled once has a 30-40% chance of re-bleeding within the same admission if not treated endoscopically. Each re-bleed carries higher mortality than the first.
- Perforation. A deep ulcer can bleed and perforate at the same time, causing peritonitis — free acid and bacteria spilling into the abdominal cavity. This converts a medical emergency into a surgical one with significant mortality.
- Missed cancer. A patient who attributes ongoing melena to "acidity" for months may be harbouring an early stomach cancer that could have been caught and cured with a timely endoscopy. By the time weight loss and difficulty swallowing appear, the disease is often advanced.
- Complications of repeated transfusions. Patients who present late often need multiple blood transfusions, each carrying its own risks: transfusion reactions, fluid overload, and iron overload with repeated episodes.
A single upper GI endoscopy done within 24 hours of symptom onset changes outcomes more than almost any other investigation in gastroenterology. It takes 15-25 minutes, is done under sedation, and in most cases both diagnoses and treats the problem.
Why Upper GI Bleeding Is a Bigger Problem in India
Four patterns in Indian clinical practice make upper GI bleeding particularly dangerous in our population.
- NSAID abuse is widespread. Diclofenac, ibuprofen, and aceclofenac are sold over the counter at every pharmacy. Patients take them daily for back pain, joint pain, and headaches — often without a prescription, without a PPI cover, and for months on end. The stomach lining accumulates damage silently until it breaks.
- H. pylori infection rates are among the highest globally. Studies from Gujarat and other Indian states report H. pylori prevalence of 60-80% in the adult population. This bacterium is the primary driver of peptic ulcer disease and gastric cancer, yet testing and eradication remain underutilised outside specialist care.
- Alcohol-related liver disease is rising. With increasing alcohol consumption across demographics, the incidence of cirrhosis and variceal bleeding is climbing. Many patients are unaware of their liver disease until a catastrophic variceal bleed.
- Late presentation is the rule, not the exception. Cultural factors — a tendency to self-treat with antacids, jeera water, and home remedies — mean that many patients arrive at hospital only when they are severely anaemic, haemodynamically unstable, or have been bleeding for days. This delay directly increases mortality.
The single most impactful change for Indian patients: treat any episode of vomiting blood or passing black tarry stool as a same-day hospital visit — not a next-week appointment.
Upper GI Bleeding Evaluation in Vadodara
Dr Samir Contractor manages patients with upper GI bleeding, peptic ulcer disease, variceal bleeding, and gastritis at Sterling Hospital, Race Course Road, Vadodara. The facility has a dedicated endoscopy suite with same-day and emergency slots, 24/7 ICU backup, and a blood bank on site.
What to bring: List of all medicines (especially painkillers, aspirin, blood thinners), any previous endoscopy or blood reports, and a responsible adult who can consent and drive you home. Come on an empty stomach in case a same-day endoscopy is needed.
Vomiting Blood or Passing Black Stool? Act Today.
Upper GI bleeding is the one condition where getting an endoscopy within 24 hours makes the biggest difference to your outcome. Sterling Hospital Vadodara offers emergency and same-day endoscopy with full ICU backup.
Frequently Asked Questions
ગુજરાતી માં પૂછાતા પ્રશ્નો (Gujarati / Hinglish FAQs)
Turant hospital javu. 108 ambulance call karo ke koi tamne emergency ma lai jaye. Lohi ni ulti — chahe taja lal hoy ke coffee jaeva kali — ae upper GI bleeding ni nishani chhe. Ghar ma rahi ne antacid leva thi kai nahi thay. Endoscopy j bleeding nu karan shodhshe ane band karshe.
Aa banne ek j vaat kahe chhe — pet ma upar thi lohi pade chhe. Ek mu thi bahaar ave chhe (hematemesis), biju neeche thi (melena). Banne hoy to bleeding vadhare chhe ane emergency ma jai ne turant endoscopy karavvi joiye.
Na. Diclofenac, Ibuprofen jaeva painkillers pet ni lining ne roj thodu thodu nukshan kare chhe. PPI dava sathe sathe painkillers pan band karva j joiye. Dard mate paracetamol safe chhe — doctor sathe vaat karo ke kai alternative chhe.
H. pylori ek bacteria chhe je pet ni lining ma rahe chhe ane ulcer kare chhe. Gujarat ma 60-70% lok ne aa infection hoy chhe. Test simple chhe — endoscopy ma biopsy, breath test, ke stool test. Positive aave to 14 divas ni antibiotic thi thik thay chhe.
Zaruri nathi ke cirrhosis j hoy. Daru pachi lohi avvu Mallory-Weiss tear (ulti thi fata), gastritis, ke varices — koi pan karan thi ho sake. Pan liver check karavu jaruri chhe. Endoscopy ane liver function test banne thava joiye. Doctor nakki karshe.
Simple diagnostic endoscopy day-care chhe — savar ma aavo, bapor sudhi ghar. Pan bleeding mate emergency endoscopy hoy to 1-3 divas admit rahevanu hoy chhe — blood test, transfusion, ane monitor karva mate. Serious hoy to vadhare pan hoy sake.