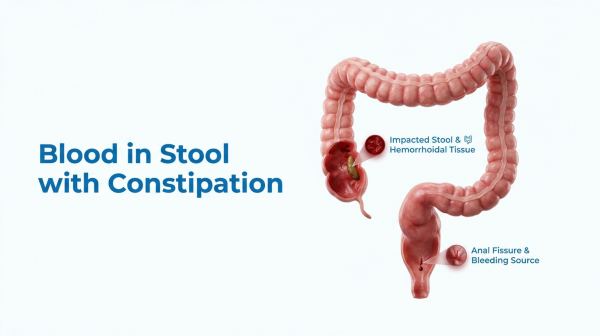
Constipation and rectal bleeding are two symptoms that patients often experience together but rarely connect. In most cases, a hard stool is the direct cause of the bleeding — it tears the anal lining or worsens piles. This guide explains the mechanism, lists the causes, flags the warning signs, and gives you a practical Indian-diet plan to break the cycle.
Quick Answers
You notice blood after a difficult bowel movement and assume the two events are unrelated. In reality, constipation is one of the most common triggers of rectal bleeding in Indian adults. Understanding how the two are linked puts you in a strong position to stop the cycle before it becomes chronic.
This page sits between our standalone guides on blood in stool (a colour-by-colour decoder) and constipation (causes and management). Here we focus specifically on the overlap — why one causes the other, when the combination signals something deeper, and how to break the pattern with simple dietary changes.
Why Constipation Causes Bleeding: The Mechanism
The Hard-Stool Cycle
The anal canal is lined by delicate tissue, and just below it sit vascular cushions (the structures that become "piles" when they swell). When stool is hard and dry, two things happen simultaneously:
- Mechanical trauma: A large, firm stool stretches and tears the anal lining on its way out. This tear is called an anal fissure. It bleeds bright red and hurts sharply.
- Vascular engorgement: Straining raises pressure inside the rectal veins. Over time, the vascular cushions swell, prolapse, and bleed on their own — these are hemorrhoids (piles). The bleeding is often painless.
Both problems feed back into the cycle. Pain from a fissure makes you dread the next bowel movement, so you hold it in, the stool dries out further, and the next attempt causes more damage. Similarly, piles that bleed after every strain grow larger with each episode.
Breaking the cycle means softening the stool. That is why dietary fibre — not medicines — is the first-line treatment for this combination.
Causes of Blood in Stool with Constipation
While fissures and piles account for the vast majority, they are not the only explanation. The table below covers the full range, from common to uncommon.
| Cause | How constipation is involved | Typical bleeding pattern | Key clue |
|---|---|---|---|
| Anal fissure | Hard stool directly tears the anal lining | Bright red streaks on stool or paper | Sharp pain during and after passing stool |
| Hemorrhoids (piles) | Straining engorges anal vascular cushions | Painless bright red drips or splash in bowl | Lump at anus, itching, long toilet sitting |
| Rectal ulcer (SRUS) | Chronic straining causes ulceration of rectal wall | Blood mixed with mucus | Feeling of incomplete evacuation |
| Colon polyps | Constipation may coexist; not directly caused by it | Dark red blood or occult (hidden) bleeding | Often silent; found on colonoscopy |
| Colorectal cancer | Tumour may narrow the passage, worsening constipation | Persistent dark blood, change in stool shape | Weight loss, anaemia, age over 40 |
| Inflammatory bowel disease | Constipation-predominant Crohn's or proctitis possible | Blood with mucus, urgency | Recurring episodes, young adults |
| Medication side effect | Iron tablets or opioid painkillers cause constipation; bleeding follows | Bright red from secondary fissure/piles | Onset matches new medication |
Fissure vs Piles: How to Tell the Difference
Patients frequently ask whether their bleeding is from a fissure or from piles. A simple guide:
- Fissure: Bright red blood with sharp, cutting pain that lasts minutes to hours after passing stool. Often triggered by a single episode of very hard stool.
- Piles: Bright red blood without significant pain. Blood drips into the bowl or is noticed when wiping. A soft lump may be felt at the anus. Develops gradually with chronic straining.
- Both together: Common. Many patients have an existing pile that bleeds after a hard stool also produces a small fissure. The clinical exam clarifies the picture.
When Constipation with Bleeding Is Concerning
Most of the time this combination is benign and fixable. But in a small number of patients, the same two symptoms point to something that needs prompt investigation. The key question is: does the bleeding make sense from the constipation, or does it have features of its own?
Polyps and Colorectal Cancer
A polyp or tumour inside the colon can cause both constipation (by narrowing the passage or altering motility) and bleeding (from the surface of the growth). The bleeding in this case is often dark red, mixed into the stool rather than on its surface, and does not go away when constipation is relieved. Other clues include unexplained weight loss, persistent change in stool calibre (pencil-thin stools), iron-deficiency anaemia, and a family history of colorectal cancer. This is why surgeons do not simply treat the constipation and assume the bleeding will stop. If the patient is over 40 or has any red flag, a colonoscopy is recommended to look inside the colon directly.
Red Flags — See a Doctor Promptly
- Bleeding that persists after constipation has been corrected for two or more weeks
- Dark red or black blood (not bright red)
- Blood mixed into the stool rather than on its surface
- Mucus along with blood
- Unintended weight loss (more than 3 kg in a month without dieting)
- Persistent change in stool shape — thin, ribbon-like, or pencil stools
- Iron-deficiency anaemia on a blood test
- Family history of colon polyps or colorectal cancer
- Age over 40 with new-onset bleeding, even if bright red
- Heavy bleeding that fills the bowl or causes dizziness
bSigns That Point to a Benign Cause
- Bright red blood only on tissue paper or stool surface
- Bleeding clearly follows a hard, difficult bowel movement
- Bleeding stops once stool becomes soft
- Small volume — a few drops, not a flow
- No weight loss, no change in appetite, no anaemia
- Young patient (under 35) with no family history
Even when all signs are reassuring, a single evaluation by a surgeon confirms the diagnosis and gives you peace of mind.
How Is It Diagnosed?
Diagnosis follows a step-by-step approach:
- History and examination: The surgeon asks about stool frequency, consistency, pain pattern, blood colour, diet, and family history. A gentle digital rectal examination checks for fissure, pile, or mass.
- Proctoscopy: A short, thin scope is passed into the lower rectum in the clinic itself. It takes under two minutes and shows internal piles, fissures, or low rectal lesions directly.
- Blood tests: A complete blood count checks for anaemia; thyroid function is tested if constipation is chronic and unexplained.
- Colonoscopy: Recommended if bleeding persists, if the patient is over 40, or if any red flag is present. The scope examines the entire colon, finds polyps, and removes them in the same sitting.
In straightforward cases — a young patient with a clear fissure after hard stool — proctoscopy alone is sufficient and no further tests are needed.
Treatment: The Fibre-First Approach
Because the root cause of bleeding in most patients is the hard stool itself, the most effective treatment starts with fixing the stool consistency. Medicines, ointments, and procedures come second.
Step 1: Indian Dietary Fibre Plan
Fibre adds bulk and moisture to stool, making it soft enough to pass without straining. The goal is 25-30 grams of fibre per day. Here is how to reach that target using everyday Indian foods:
| Meal | Fibre-rich choices | What to reduce |
|---|---|---|
| Breakfast | Whole wheat paratha with curd, or poha with vegetables, or oats chilla. Add a banana or papaya. | Maida bread, biscuits, instant noodles |
| Lunch | 2 whole wheat roti + dal (moong, masoor, or chana) + 1 bowl green sabzi (bhindi, palak, lauki) + salad (cucumber, carrot, radish) | White rice alone without dal or sabzi, fried snacks |
| Evening | Sprouts chaat, roasted chana, a seasonal fruit (guava, apple, pear with skin) | Samosa, vada pav, packaged chips |
| Dinner | 2 roti + lighter sabzi + small bowl dal or kadhi. Add a handful of salad. | Heavy paneer gravy, excessive ghee, late-night snacking |
| Before bed | 1 teaspoon sat isabgol (psyllium husk) in a full glass of warm water or milk | Tea or coffee late at night (dehydrates stool) |
Water is just as important as fibre. Fibre absorbs water to form a soft gel. Without enough fluids (at least 8-10 glasses per day), extra fibre can actually make constipation worse. Drink water throughout the day, not just at mealtimes.
Step 2: Sat Isabgol (Psyllium Husk)
Sat isabgol is the single most effective fibre supplement available in India. It is natural, inexpensive, and available at every medical store. Take 1-2 teaspoons in a full glass of water or warm milk at bedtime. It forms a gel that softens stool overnight, and most patients notice a difference within 2-3 days. Continue daily for at least 4-6 weeks while the fissure or piles heal.
Step 3: Topical Treatment and Sitz Baths
For anal fissure: a warm sitz bath (sitting in warm water for 10 minutes, twice daily) relaxes the anal sphincter and promotes healing. Your surgeon may prescribe a topical ointment containing a muscle relaxant (diltiazem or glyceryl trinitrate) to reduce spasm and pain.
For piles: topical creams reduce swelling and itching. A stool softener (liquid paraffin or lactulose) may be added short-term while dietary changes take effect.
Step 4: When Surgery Is Needed
Surgery is considered only when the above measures fail after an adequate trial (usually 6-8 weeks):
- Chronic anal fissure: A small day-care procedure (lateral internal sphincterotomy) cures the fissure by releasing the tight muscle. Recovery takes about a week. Read more on our fissure surgery page.
- Grade 3-4 hemorrhoids: Laser hemorrhoidoplasty or stapler hemorrhoidopexy provides lasting relief with minimal pain. Both are day-care procedures. Details on our hemorrhoid surgery page.
- Polyps or early cancer: Polyps found on colonoscopy are removed during the procedure itself. If cancer is detected, a structured treatment plan is discussed — early-stage colorectal cancer has excellent outcomes when caught early.
What Happens If You Ignore It?
Leaving the constipation-bleeding cycle untreated has real consequences:
- Acute fissure becomes chronic: A fresh tear that could heal in 2 weeks with fibre alone becomes a deep, scarred chronic fissure that requires surgery.
- Early piles progress to advanced grades: Grade 1 internal piles that respond to diet can advance to grade 3-4 prolapsing piles that need a procedure.
- Iron-deficiency anaemia: Daily small-volume bleeding adds up. Over months, haemoglobin drops, causing fatigue, breathlessness, and poor concentration — often attributed to "stress" instead of the actual bleeding.
- A polyp is missed: If the bleeding is assumed to be from constipation alone without a proper check, a polyp can grow undetected for years. Polyps are the precursors of most colorectal cancers.
- Quality of life drops: Fear of pain leads to stool-holding, which leads to harder stool, more bleeding, and a cycle of anxiety around every bathroom visit.
The cost of one evaluation is far lower than the cost of treating an advanced condition that could have been caught early.
Why This Matters in India
- Constipation is extremely common: Studies estimate 15-22% of Indian adults report chronic constipation, driven by low-fibre processed foods, inadequate water intake, and sedentary urban lifestyles.
- Piles and fissures are under-treated: Many patients tolerate bleeding for months or years, using home remedies or over-the-counter ointments, before seeking a surgeon.
- Colorectal cancer is rising: India is seeing a steady increase in colorectal cancer, particularly in urban populations under 50. Early screening with colonoscopy can catch polyps before they turn cancerous.
- Traditional Indian diets are fibre-rich — but modern eating is not: A dal-roti-sabzi meal provides excellent fibre. The shift toward maida-based foods, packaged snacks, and low-vegetable diets is directly linked to the rise in constipation-related bleeding.
- Sat isabgol is widely available: India has one of the best natural fibre supplements in the world — psyllium husk — grown domestically and available at every chemist for a few rupees. Most patients do not need expensive imported supplements.
Consult Dr Samir Contractor in Vadodara
If you are experiencing blood in stool with constipation — whether it is the first episode or a recurring problem — a single consultation can identify the cause, rule out anything serious, and give you a clear treatment plan.
Constipation with Bleeding? Get Checked Once.
A single consultation can rule out serious conditions and give you a clear plan — often starting with simple dietary changes.
Frequently Asked Questions
Patients Also Ask (Gujarati / Hinglish)
A: Pahela stool ne naram karvo — roti, dal, sabzi, fruit vadharo ane roj ek chamchi sat isabgol pani sathe lo. Jyare potho naram thase, lathi apne aap bandh thase. Jo bandh na thay to doctor ne batavo.
A: Moat bhag na cases ma aa fissure ke piles hoy che — bright red blood, stool pass karva thi. Cancer ma blood dark hoy, stool ni andar mix hoy, ane weight loss thay. Doctor ni ek visit thi khbar padi jay.
A: Na, sat isabgol natural fibre che. Roj levi safe che — bas sathe puri glass pani pivanu. Aa laxative nathi, aa stool ne naram kare che naturally.
A: General surgeon athva piles specialist pase javo. Dr Samir Contractor, Sterling Hospital Vadodara — piles, fissure, ane colon ni problem ma experienced che. Proctoscopy clinic ma j thay che, 2 minute ma.
A: Jyare diet fix karya pacchi pan blood bandh na thay, umar 40 thi upar hoy, ya family ma cancer hoy to colonoscopy recommend thay. Nahi to pehla proctoscopy thi j answer mali jay.
A: Baby ne direct asar nathi thati. Pregnancy ma constipation common che ane aa thi fissure thay. Fibre, pani, ane sat isabgol safe che pregnancy ma. Pan doctor ne janna jaroor karo.