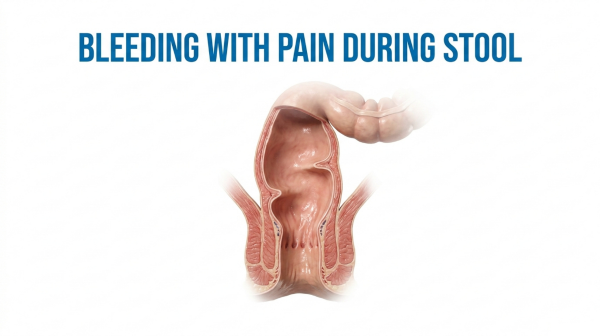
In short: Bright red bleeding accompanied by sharp pain during a bowel movement is most commonly caused by an anal fissure — a small tear in the anal lining. Unlike painless rectal bleeding (which usually points to internal hemorrhoids), the combination of pain + bleeding narrows the likely diagnosis significantly and responds well to early treatment.
Quick Answers
Why Does It Bleed and Hurt When You Pass Stool?
When bleeding and pain occur together during a bowel movement, the anal canal is almost always the source. The anal lining is richly supplied with sensory nerve endings (somatic nerves), which is why injuries here produce immediate, sharp pain — unlike the relatively pain-free internal hemorrhoidal zone higher up.
The most straightforward explanation: hard or large stool stretches the anal tissue beyond its elastic limit, creating a linear tear. That tear bleeds on contact and triggers a spasm of the internal anal sphincter, which further reduces blood supply and slows healing. This cycle — tear, spasm, poor healing, re-tear — is what turns an acute fissure into a chronic one.
Causes of Bleeding with Pain During Stool
1. Anal Fissure (Most Common)
An anal fissure accounts for the vast majority of cases where patients report the specific combination of bright red bleeding plus sharp pain during defecation. Key features include:
- Tearing or cutting pain that starts during the bowel movement and may last 30 minutes to several hours afterward
- Bright red blood, usually a small amount, on the stool surface or tissue paper
- Pain triggered or worsened by constipation and hard stool
- A visible crack or sentinel skin tag at the anal margin in chronic cases
Fissures are overwhelmingly located at the posterior midline of the anal canal. An off-midline fissure raises suspicion for other conditions such as Crohn's disease, tuberculosis, or HIV-related ulceration and warrants further investigation.
2. Thrombosed Hemorrhoids (Piles)
When a blood clot forms inside an external hemorrhoid, it produces a firm, bluish, extremely tender lump near the anus. Bleeding occurs if the overlying skin breaks open. The pain is constant and worsens with sitting, unlike fissure pain which peaks during and shortly after defecation.
3. Perianal Abscess
A perianal abscess is an infection-filled cavity near the anus. It causes throbbing, escalating pain that does not depend on bowel movements, often accompanied by fever. If the abscess ruptures or is drained, blood-tinged pus may appear with the stool. This requires urgent surgical drainage.
4. Proctitis
Inflammation of the rectal lining — from inflammatory bowel disease (IBD), infections, or radiation — can cause painful bleeding with mucus. The pain is typically a deeper rectal discomfort rather than the sharp, localized anal pain of a fissure.
Pain + Bleeding: How to Tell If It Is a Fissure or Something Else
The character of both the pain and the bleeding offers reliable diagnostic clues before any examination:
- Fissure: Sharp, knife-like pain during stool → burning ache for 30 min–2 hrs → relief until next movement. Bleeding is small-volume, bright red.
- Thrombosed pile: Constant, pressure-type pain + visible swollen lump. Bleeding only if skin ruptures.
- Abscess: Throbbing pain that worsens over hours/days regardless of stool. Fever and swelling are common.
- Proctitis: Deep rectal ache, urgency, mucus mixed with blood. Pain is not sharply tied to the act of passing stool.
Important distinction: If you experience painless bright red bleeding, the pattern points toward a different set of causes (primarily internal hemorrhoids). That symptom profile is covered in detail on our painless rectal bleeding page.
Red Flags — See a Doctor Urgently
- Heavy bleeding that fills the toilet bowl or causes dizziness
- Dark or maroon-coloured blood (may indicate a source higher in the GI tract)
- Fever, pus, or foul-smelling discharge (suggests abscess or infection)
- Unintended weight loss or change in bowel habits lasting more than 4 weeks
- Painful bleeding in patients over 50 with no prior history (colorectal screening needed)
- Pain and bleeding that worsen progressively despite 2 weeks of home measures
Signs That Suggest a Straightforward Fissure
- Pain is strictly linked to passing stool and subsides between movements
- Bleeding is small-volume, bright red, and on the surface (not mixed into stool)
- Symptoms started after a period of constipation, hard stool, or straining
- No fever, no lump, no discharge
- Age under 50 with no family history of colorectal disease
Even with these reassuring features, a specialist visit is recommended if symptoms persist beyond 2–3 weeks.
How Is the Cause Diagnosed?
Diagnosis is primarily clinical and begins with a focused history and gentle visual inspection:
- History: Character of pain (sharp vs. throbbing), timing relative to stool, duration, associated symptoms (fever, weight loss, mucus), and bowel habit
- Visual inspection: In most fissure cases, the tear is visible simply by gently parting the buttocks. A thrombosed pile presents as an obvious bluish swelling.
- Digital rectal examination: Often deferred in acute fissure due to severe sphincter spasm and pain. Performed under local anaesthesia if needed.
- Proctoscopy / Anoscopy: Allows direct visualization of the lower anal canal and distal rectum. Essential to rule out internal hemorrhoids or proctitis.
- Colonoscopy: Reserved for patients with red-flag features, age over 50, family history of colorectal cancer, or atypical fissure presentation.
Treatment Options
Conservative (First-Line) Management
- Dietary fibre: 25–35 g/day from whole grains, vegetables, fruits, and psyllium husk (isabgol)
- Water intake: At least 2.5–3 litres daily to soften stool naturally
- Sitz baths: Warm water soaks for 10–15 minutes, 2–3 times a day, especially after bowel movements. Relieves sphincter spasm.
- Stool softeners: Osmotic laxatives (lactulose) or bulk-forming agents as needed
- Topical agents: GTN (glyceryl trinitrate 0.2%) ointment or diltiazem cream to relax the sphincter and improve blood flow
- Pain management: Topical lignocaine gel for temporary relief before bowel movements
Approximately 60–70% of acute fissures heal with 6–8 weeks of consistent conservative therapy.
Surgical Treatment (When Conservative Measures Fail)
- Lateral Internal Sphincterotomy (LIS): The gold standard for chronic fissures. A small, controlled cut in the internal sphincter muscle reduces spasm permanently. Healing rate exceeds 95%.
- Botulinum toxin injection: A less invasive alternative that temporarily paralyzes the sphincter. Recurrence rates are higher than LIS.
- Hemorrhoidectomy: If thrombosed or prolapsed hemorrhoids are the cause, surgical removal may be indicated.
- Abscess drainage: Incision and drainage under anaesthesia for confirmed perianal abscess. Fistula assessment follows.
What Happens If You Ignore Bleeding with Pain During Stool?
- Acute fissure becomes chronic: After 6–8 weeks without healing, the fissure margins fibrose, forming a sentinel pile and hypertrophied anal papilla. Chronic fissures rarely heal without intervention.
- Fear-driven constipation cycle: Many patients begin avoiding stool due to anticipated pain, which leads to harder stool, worsening the tear — a self-reinforcing cycle.
- Abscess progression: An untreated perianal abscess can spread along tissue planes, forming a fistula or causing sepsis.
- Missed serious pathology: In rare cases, what appears to be a simple fissure may mask an underlying condition such as Crohn's disease, anal tuberculosis, or malignancy. Early evaluation catches these.
- Chronic pain and quality of life: Ongoing anal pain affects sitting, working, and daily activities, often leading to anxiety around bowel movements.
Why This Matters in India
Anal fissure and related conditions are extremely common across India, yet patients frequently delay seeking help due to embarrassment and stigma around anorectal problems. Key factors relevant to the Indian context:
- High constipation prevalence: Diets low in fibre, inadequate water intake, and sedentary lifestyles contribute to constipation — the leading trigger for anal fissures — across urban and rural populations
- Cultural hesitancy: Many patients, especially women, avoid discussing rectal symptoms for years. By the time they consult, fissures have often become chronic
- Self-medication risks: Over-the-counter steroid creams and unregulated Ayurvedic preparations are frequently used without diagnosis, sometimes worsening the condition or masking infections
- Misconception that all rectal bleeding = piles: In India, "piles" is commonly used as a catch-all term. Patients and even some general practitioners assume bleeding = piles, which delays correct diagnosis and appropriate treatment
- Access to specialists: In Gujarat and across India, proctology expertise is available at major centres. Early consultation with a qualified surgeon prevents complications and reduces overall treatment cost
Consult Dr Samir Contractor in Vadodara
If you are experiencing bleeding with pain during stool, an accurate diagnosis is the first step toward relief. Dr Samir Contractor offers confidential, thorough anorectal evaluation at Sterling Hospital, Vadodara.
Need advice?
Frequently Asked Questions
Gujarati & Hinglish FAQs — સ્થાનિક ભાષામાં
જવાબ: મોટા ભાગે આ ફિશર (ગુદામાં ચીરો) ને કારણે થાય છે. ગરમ પાણીમાં બેસવું, વધુ ફાયબર ખાવું, અને ડૉક્ટરની સલાહ લેવી.
જવાબ: દુખાવા વગરનું લોહી સામાન્ય રીતે અંદરના મસા (piles) સૂચવે છે, જ્યારે દુખાવા સાથેનું લોહી ફિશર તરફ ઈશારો કરે છે.
Jawaab: Yeh zyaadatar fissure ke kaaran hota hai. Garam paani mein baithna, fibre wala khana khana, aur specialist se milna zaruri hai.
જવાબ: ઓપરેશન પછી ફરી ફિશર થવાની શક્યતા ઘણી ઓછી છે (2-5%). યોગ્ય આહાર જાળવવાથી રિસ્ક ઘટે છે.
Jawaab: Zyaadatar haan, constipation sabse bada kaaran hai. Lekin diarrhoea, pregnancy, aur zyaada strain karna bhi fissure bana sakta hai.
જવાબ: ડૉ. સમીર કોન્ટ્રેક્ટર, સ્ટર્લિંગ હોસ્પિટલ, વડોદરા — 25+ વર્ષનો અનુભવ અને 8,000+ સર્જરી.