Lower GI bleeding is any bleeding that originates below the ligament of Treitz - from the small
bowel, colon, rectum, or anus. It ranges from minor hemorrhoidal spotting to life-threatening
haemorrhage, and always warrants proper evaluation.
This clinical guide by Dr Samir Contractor covers every major cause, the diagnostic pathway,
treatment approaches, and when to seek emergency care.
Quick Answers
What Is Lower GI Bleeding?
Lower gastrointestinal (GI) bleeding refers to blood loss originating from the portion of the digestive tract that lies beyond the ligament of Treitz - the anatomical landmark where the duodenum meets the jejunum. Everything proximal to this point (oesophagus, stomach, duodenum) falls under upper GI bleeding.
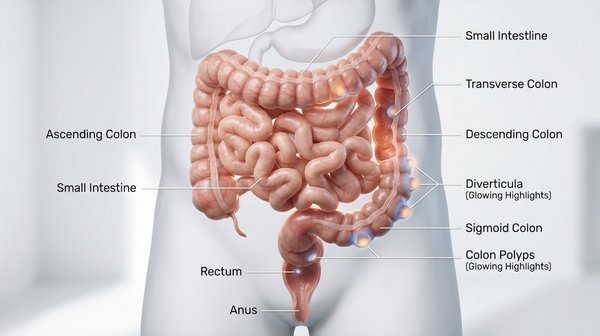
In practical terms, the lower GI tract includes the jejunum, ileum, caecum, ascending colon, transverse colon, descending colon, sigmoid colon, rectum, and anal canal. The vast majority of clinically significant lower GI bleeding arises from the colon, rectum, or anus.
Lower GI bleeding accounts for roughly 20–30% of all GI bleeding presentations. While it tends to carry a lower mortality rate than upper GI bleeding (approximately 2–4% versus 6–10%), massive lower GI haemorrhage can be life-threatening and demands urgent intervention.
How Does Lower GI Bleeding Present?
The hallmark presentation is hematochezia - the passage of bright red or maroon-coloured blood through the rectum. Depending on the source and severity, patients may notice:
- Bright red blood on toilet paper, on the stool surface, or dripping into the toilet bowl
- Blood mixed within the stool, giving it a maroon appearance
- Large clots with or without stool
- Occult (hidden) blood detected only on laboratory testing, with no visible bleeding
- Iron-deficiency anaemia from slow chronic blood loss - fatigue, pallor, breathlessness
Important distinction: dark, tarry stools (melena) typically suggest an upper GI source. However, a very slow bleed from the right colon can occasionally produce melena, and a very brisk upper GI haemorrhage can produce bright red blood per rectum. Context matters - and that is why proper evaluation is indispensable.
Causes of Lower GI Bleeding
The causes span a wide spectrum, from entirely benign conditions to potentially fatal pathology. Organised by frequency and clinical importance:
1. Hemorrhoids (Piles)
The single most common cause of rectal bleeding, especially in adults under 50. Internal hemorrhoids produce painless bright red bleeding - often noticed as dripping after a bowel movement. While usually not dangerous, they can cause significant anaemia if ignored over months or years. Surgical options exist for advanced grades.
2. Anal Fissure
A small tear in the anal lining, typically caused by passing hard stools. Produces sharp pain during defecation along with a streak of bright red blood. Most fissures heal with dietary changes and topical treatment; chronic fissures may need surgery.
3. Diverticular Disease
Diverticula are small pouches that form in the colonic wall, most often in the sigmoid colon. Diverticular bleeding is the most common cause of massive lower GI bleeding in patients over 60. It is characteristically painless and can be profuse - but stops spontaneously in about 75–80% of cases. The risk increases with age, NSAID use, and anticoagulant therapy.
4. Colorectal Polyps
Polyps are growths on the inner lining of the colon or rectum. Most are benign but some carry malignant potential (adenomatous polyps). Bleeding from polyps is usually occult or low-volume. Detection and removal during colonoscopy (polypectomy) is both diagnostic and preventive - removing pre-cancerous polyps prevents progression to colorectal cancer.
5. Colorectal Cancer
Bleeding - either visible or occult - is one of the most important presenting features of colorectal cancer. The bleeding pattern depends on the tumour location: right-sided tumours often cause occult bleeding and anaemia, while left-sided and rectal tumours tend to produce visible blood in the stool. Any new-onset rectal bleeding in a patient over 40, or any change in bowel habit accompanying bleeding, demands a colonoscopy.
6. Angiodysplasia (Arteriovenous Malformations)
Abnormal, fragile blood vessels in the colonic wall - most commonly found in the caecum and right colon. These account for approximately 3–12% of lower GI bleeding cases and are more prevalent in elderly patients and those with chronic kidney disease. Bleeding is usually low-grade and intermittent but can occasionally be severe.
7. Colitis (Inflammatory, Infectious, Ischaemic)
Inflammation of the colon from various causes can produce bloody diarrhoea:
- Inflammatory bowel disease (IBD) - ulcerative colitis and Crohn's disease cause chronic, relapsing bloody diarrhoea with mucus
- Infectious colitis - bacterial infections (Salmonella, Shigella, E. coli, C. difficile) produce acute bloody diarrhoea
- Ischaemic colitis - reduced blood flow to the colon, most common in elderly patients with cardiovascular disease, presents with sudden abdominal pain and bloody stools
Other Causes
- Radiation proctitis (following pelvic radiotherapy)
- Solitary rectal ulcer syndrome
- Meckel's diverticulum (a common cause of lower GI bleeding in children and young adults)
- Post-polypectomy bleeding (a recognised complication occurring 1–2 weeks after colonoscopic polypectomy)
- Anticoagulant and antiplatelet medications (unmask or worsen bleeding from any underlying source)
Acute vs. Chronic Lower GI Bleeding
| Feature | Acute Lower GI Bleeding | Chronic Lower GI Bleeding |
|---|---|---|
| Onset | Sudden, often dramatic | Gradual, over weeks to months |
| Volume | Moderate to massive | Small, often occult |
| Presentation | Bright red blood, haemodynamic instability | Iron-deficiency anaemia, fatigue, positive FOBT |
| Common causes | Diverticular disease, angiodysplasia | Hemorrhoids, polyps, colorectal cancer |
| Urgency | Emergency evaluation required | Elective colonoscopy within weeks |
Red Flags - Seek Emergency Care Immediately
- Passing large quantities of blood - soaking through clothing or filling the toilet bowl
- Dizziness, lightheadedness, or fainting
- Rapid heart rate (tachycardia) or feeling your heart pounding
- Cold, clammy skin or confusion - signs of shock
- Severe abdominal pain accompanying bleeding
- Bleeding while on blood thinners (warfarin, heparin, DOACs) or dual antiplatelet therapy
- Bleeding accompanied by high fever (suggests severe infectious or ischaemic colitis)
- Unexplained weight loss combined with rectal bleeding (raises suspicion for malignancy)
When Is Lower GI Bleeding Likely Less Serious?
- Small amounts of bright red blood only on wiping - usually hemorrhoidal
- Blood associated with painful bowel movements and hard stools - suggests anal fissure
- Single episode, small volume, no other symptoms, young and healthy individual
- Known stable hemorrhoids with a typical bleeding pattern
Even in these scenarios, a clinical evaluation is recommended - especially for anyone over 40 or with a family history of colorectal cancer.
Diagnosis of Lower GI Bleeding
The diagnostic approach depends on the severity and acuity of bleeding:
Colonoscopy - The Primary Tool
Colonoscopy is the gold standard for evaluating lower GI bleeding. It allows direct visualisation of the entire colon and rectum, identification of the bleeding source, biopsy of suspicious lesions, and therapeutic intervention (clipping, cauterisation, injection, polypectomy) - all in a single procedure.
For acute bleeding, urgent colonoscopy (performed within 12–24 hours after bowel preparation and haemodynamic stabilisation) improves diagnostic yield and enables immediate treatment.
CT Angiography - For Acute Massive Bleeding
When bleeding is too brisk for safe colonoscopy, CT angiography can rapidly detect the bleeding site if the rate exceeds approximately 0.3–0.5 mL per minute. It is widely available, fast, and non-invasive - making it an excellent first step in haemodynamically unstable patients before deciding on angiographic embolisation or surgery.
Other Diagnostic Tools
- Tagged red blood cell scan - highly sensitive for detecting intermittent, slow bleeding (rates as low as 0.1 mL/min) but lacks precise localisation
- Capsule endoscopy - useful for small-bowel bleeding that colonoscopy and upper endoscopy cannot explain
- Anoscopy / proctoscopy - simple bedside examination to evaluate hemorrhoidal and anal canal pathology
- Stool studies and blood tests - complete blood count, coagulation profile, blood typing, stool cultures when infection is suspected
Treatment of Lower GI Bleeding
Resuscitation and Stabilisation
The immediate priority in acute bleeding is haemodynamic stabilisation: intravenous fluid resuscitation, blood transfusion when haemoglobin drops below critical levels, and correction of any coagulopathy. Anticoagulants may need to be held or reversed after discussion with the prescribing team.
Endoscopic Treatment
Colonoscopy is both diagnostic and therapeutic. Techniques include mechanical clipping of a visible bleeding vessel, thermal cauterisation (bipolar or argon plasma coagulation), and injection of adrenaline or sclerosants. Polypectomy removes bleeding polyps. These methods resolve bleeding in the majority of cases.
Angiographic Embolisation
Interventional radiology can catheterise the feeding artery and embolise the bleeding vessel using coils or gel foam. This is reserved for patients with massive bleeding that cannot be controlled endoscopically, or when the bleeding source is identified on CT angiography.
Surgery
Surgical intervention - typically segmental colectomy - is reserved for patients with life-threatening bleeding that fails endoscopic and angiographic control, recurrent bleeding from a localised source, or confirmed colorectal cancer requiring resection.
Cause-Specific Treatment
- Hemorrhoids: dietary modification, rubber band ligation, hemorrhoidectomy
- Anal fissure: fibre supplementation, topical GTN/diltiazem, lateral internal sphincterotomy for chronic fissures
- IBD: 5-ASA agents, corticosteroids, immunomodulators, biologics
- Infectious colitis: appropriate antibiotics, supportive care
- Iron-deficiency anaemia from chronic bleeding: oral or IV iron supplementation alongside treatment of the source
What Happens If Lower GI Bleeding Is Ignored?
- Missed colorectal cancer: early-stage colorectal cancer is highly curable (90%+ five-year survival for stage I). Ignoring bleeding allows time for progression to advanced, less treatable stages.
- Severe iron-deficiency anaemia: chronic unaddressed bleeding steadily depletes iron stores, causing debilitating fatigue, breathlessness, heart strain, and cognitive effects.
- Emergency surgery: a minor source that could have been treated electively via colonoscopy may eventually cause a massive haemorrhage requiring emergency surgery with higher complication rates.
- Progression of treatable conditions: polyps grow, hemorrhoids worsen, and IBD flares become harder to control without timely intervention.
- Psychological burden: unexplained bleeding causes anxiety. Proper diagnosis provides clarity and a treatment plan.
Lower GI Bleeding in the Indian Context
Several factors make lower GI bleeding a particularly important clinical problem in India:
- Rising colorectal cancer incidence: India has seen a steady increase in colorectal cancer, especially in urban populations. The average age at diagnosis is lower in India than in Western countries - making evaluation of rectal bleeding in younger patients essential.
- High prevalence of hemorrhoids: dietary patterns, sedentary lifestyles, and chronic constipation contribute to a very high burden of hemorrhoidal disease across all age groups.
- Infectious colitis: bacterial dysentery (Shigella, E. coli), amoebic colitis, and tuberculosis of the colon remain significant causes of bloody diarrhoea in India, unlike in Western populations where they are uncommon.
- Delayed presentation: cultural hesitation around discussing rectal symptoms, limited access to colonoscopy in rural areas, and reliance on empirical treatment without investigation all contribute to delayed diagnosis.
- Growing colonoscopy access: major centres like Vadodara now have excellent endoscopy infrastructure, making timely diagnosis and treatment accessible for patients across Gujarat.
- Anticoagulant use: with an ageing population and increasing cardiovascular disease, more Indian patients are on blood thinners - amplifying the risk and severity of GI bleeding.
Consult Dr Samir Contractor in Vadodara
If you or a family member is experiencing lower GI bleeding - whether it is a small amount of blood on wiping or a more alarming episode - get a proper clinical evaluation. Early diagnosis saves lives.
Need a clinical evaluation?
Frequently Asked Questions About Lower GI Bleeding
?? Gujarati & Hinglish FAQs - Lower GI Bleeding
A: તરત જ ડૉક્ટરને મળો. અમુક વખતે તે હરસ હોય શકે છે, પણ કોલોનોસ્કોપી કરાવવી જરૂરી છે.
A: Hamesha serious nahi hota - bahut baar piles ya fissure hota hai. Lekin cancer bhi aise hi start hota hai, isliye check karwana zaroori hai.
A: ના, સેડેશન હેઠળ દુખાવો નથી થતો. માત્ર આગલા દિવસે દવાઓ લેવી પડે છે.
A: Ghar pe fark batana mushkil hai - dono mein bright red blood aa sakta hai. Isliye doctor se milke colonoscopy karwana sabse safe hai.
A: હા, સ્ટર્લિંગ હોસ્પિટલમાં ડૉ. સમીર કોન્ટ્રેક્ટર પાસે આધુનિક સુવિધા સાથે કોલોનોસ્કોપી થાય છે.
A: Blood thinner band mat karo apne aap se - pehle doctor se milo. Doctor bleeding ka source dhundhenge aur thinner adjust karenge safely.