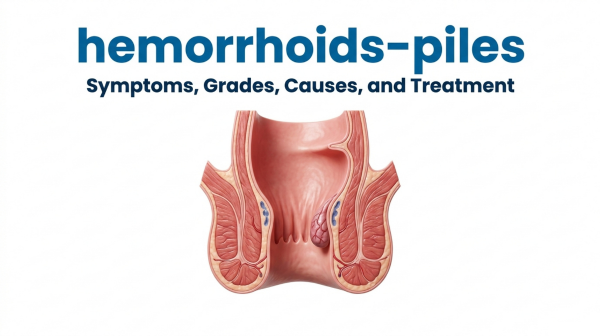
Piles are swollen blood-vessel cushions inside or around the anus. They are extremely common, usually harmless, and almost always treatable — but the right treatment depends on the grade. This page explains every grade, when to worry, and which options are available in Vadodara.
Quick Answer
Introduction
Hemorrhoids known in everyday language as piles and in Gujarati as bavasir or mulvyadh are one of the most common conditions in the world. Roughly half of all adults experience symptoms from piles at some point, yet most delay seeking help because of embarrassment, fear of surgery, or the hope that home remedies will be enough.
This page gives you a complete picture: what piles actually are, how they are graded, what causes them, which symptoms need attention, and the full range of treatment from dietary changes to day-care laser surgery. If you arrived here from our rectal bleeding or blood in stool page, you are in the right place — piles are the single most common cause of both.
What Are Hemorrhoids?
The anal canal contains three natural vascular cushions — clusters of tiny blood vessels, smooth muscle, and connective tissue — that help with continence and fine control of stool passage. When these cushions become enlarged, engorged, or displaced downward, they are called hemorrhoids. The word "piles" is simply the lay English term; both mean the same thing.
Internal vs External Hemorrhoids
Internal hemorrhoids sit above the dentate line, inside the anal canal. They are covered by a mucous membrane that has very few pain fibres, which is why internal piles usually bleed without pain. They are the type that prolapse (come out during straining).
External hemorrhoids sit below the dentate line, around the anal opening. They are covered by skin rich in nerve endings, which is why external piles — and especially thrombosed external piles — can be intensely painful, even without bleeding.
Grading System
Internal hemorrhoids are classified into four grades based on how far they prolapse. The grade determines the treatment.
| Grade | What happens | Typical symptoms | Usual treatment |
|---|---|---|---|
| I | Cushion is enlarged but does not come out | Painless bleeding after stool | Fibre, water, topical treatment |
| II | Comes out during straining, goes back in on its own | Bleeding, slight prolapse, mucous | Banding, sclerotherapy, laser (if recurrent) |
| III | Comes out and must be pushed back manually | Prolapse, bleeding, soiling, discomfort | Laser, stapler, or conventional surgery |
| IV | Permanently prolapsed, cannot be pushed back | Constant prolapse, heavy bleeding, pain, hygiene difficulty | Stapler or conventional excision surgery |
Thrombosed external hemorrhoid: Not part of the grading system above. This is a painful, firm, bluish lump at the anal verge caused by a blood clot inside an external pile. It can occur at any time, is very painful, and is best treated by incision and drainage within 48–72 hours.
Causes and Risk Factors
Piles develop when pressure on the anal cushions increases chronically. The usual contributors include:
- Chronic constipation and straining. The single biggest risk factor. Hard stools require prolonged pushing, which engorges the cushions.
- Low-fibre diet. Refined flour (maida), white rice without dal, and minimal vegetables lead to hard, small-volume stools.
- Inadequate water intake. Especially common in Gujarat during summer.
- Prolonged toilet sitting. Reading, scrolling, or straining for more than 5 minutes disrupts venous return.
- Sedentary lifestyle. Long hours of desk work or driving increase pelvic congestion.
- Pregnancy. The growing uterus presses on pelvic veins, and hormonal changes soften connective tissue. Piles are very common in the third trimester.
- Obesity. Excess abdominal fat increases intra-abdominal pressure.
- Heavy lifting. Repeated straining (gym, manual labour) raises abdominal pressure.
- Ageing. Connective tissue weakens over time, allowing cushions to slip downward.
- Chronic diarrhoea. Frequent liquid stools irritate the anal canal and keep cushions swollen.
Symptoms
The symptoms you experience depend on whether the piles are internal or external and what grade they are.
Internal Piles
- Painless bright-red bleeding: blood drips into the toilet bowl or coats the stool. This is the hallmark symptom.
- Prolapse: a soft lump that comes out during straining and may or may not go back in.
- Mucous discharge: a clear, slimy fluid that stains undergarments.
- Itching (pruritus ani): caused by mucous discharge irritating perianal skin.
- Sense of incomplete evacuation: the prolapse can make you feel like stool is still present.
External Piles
- Painful swelling at the anal verge, especially if thrombosed.
- Skin tags: small flaps of skin that remain after a previous external pile resolves.
- Difficulty with hygiene: skin tags and swelling make cleaning difficult.
See a Doctor If You Notice
- Bleeding that does not stop with conservative measures
- A prolapse that cannot be pushed back or is very painful
- Blood that is dark red, mixed into stool, or accompanied by weight loss this pattern is not typical of piles
- A new change in bowel habit alongside bleeding
- Age over 40 with first episode of bleeding
- Severe sudden anal pain with a firm lump (thrombosed pile)
Usually Manageable at Home (Short Term)
- Occasional small amount of bright red blood with hard stool
- Known Grade I/II piles with a mild flare
- Mild itching that responds to warm-water sitz baths
- Piles during pregnancy that are not thrombosed or prolapsed
Home management is a bridge, not a cure. If symptoms return more than twice in 6 months, a clinical evaluation is due.
Diagnosis
A clinical examination is usually all that is needed. Dr Samir Contractor performs a digital rectal examination followed by a proctoscopy — a short scope that visualises the anal canal and lower rectum. This takes under 5 minutes, is done in the OPD, and tells you the exact grade of your piles.
If the bleeding pattern suggests a source higher up — dark blood, mixed blood, weight loss, change in bowel habit a colonoscopy is recommended to rule out polyps or other conditions.
Treatment Options
Conservative Treatment (Grade I, Early Grade II)
- Fibre: 25–30 g/day from whole-wheat roti, chhilka wali daal, fruits with skin, vegetables.
- Water: 2.5–3 L per day.
- Stool softeners for short courses (ispaghula husk, lactulose).
- Sitz baths: warm-water soaks for 10–15 minutes, 2–3 times/day.
- Topical ointments and suppositories containing local anaesthetic, steroids, or astringents. Use for 7–10 days only prolonged use can thin the skin.
- Avoiding straining: do not spend more than 5 minutes on the toilet. Do not scroll your phone.
Office Procedures (Grade I–II)
- Rubber-band ligation (RBL): A small rubber ring is placed around the base of the internal pile to cut off its blood supply. It shrivels and falls off in 5–7 days. No anaesthesia needed.
- Sclerotherapy: A chemical is injected into the pile to shrink it. Best for small Grade I piles with bleeding.
- Infrared coagulation (IRC): A beam of infrared light coagulates the tissue. Useful for small, bleeding internal piles.
Laser Hemorrhoidectomy (Grade II–III)
A diode laser fibre is used to shrink the hemorrhoidal tissue from within. Advantages include less post-operative pain, less blood loss, and faster return to work (typically 3–5 days). It is not suitable for very large Grade IV piles with significant external component.
Stapler Hemorrhoidopexy (Grade III–IV)
A circular stapling device lifts the prolapsed cushions back into position and cuts off their excess blood supply. The procedure takes about 30 minutes under spinal or general anaesthesia. It carries less pain than traditional excision but slightly higher long-term recurrence in some studies.
Conventional Excision Hemorrhoidectomy (Grade III–IV)
The gold standard for advanced piles. The enlarged cushion is excised under direct vision. Post-operative pain is higher, but long-term cure rate is the best of all techniques. Modern wound-care protocols and pain management have improved recovery significantly.
Thrombosed External Pile — Emergency
A thrombosed external pile that presents within 48–72 hours is best treated by incision and clot evacuation — a minor procedure done under local anaesthesia in the clinic. After 72 hours, the clot begins organising and conservative treatment (sitz baths + analgesia) is usually preferred.
What Happens If Piles Are Ignored?
- Grade progression. Grade I piles left untreated with continued constipation often progress to Grade II, then III. Early treatment is simpler, cheaper, and more comfortable.
- Chronic anaemia. Daily small bleeds can cause iron-deficiency anaemia — fatigue, pallor, and breathlessness on exertion.
- Thrombosis. A prolapsed internal pile can become trapped (strangulated), clot, and cause severe pain requiring emergency treatment.
- Skin problems. Chronic mucous discharge leads to perianal dermatitis, itching, and breakdown of the skin around the anus.
- Missed coexisting pathology. Self-treating "piles" for years without evaluation risks missing a fissure, fistula, or rarely a rectal tumour that was there all along.
Why This Matters in India
Piles are arguably the most under-treated surgical condition in India. Millions of adults tolerate years of bleeding because of three misconceptions.
- "Piles will go away on their own." Grade I may settle temporarily, but without fixing the cause (low fibre, straining), they return and progress.
- "Surgery means weeks of bed rest." With laser and stapler techniques, most patients are back at work in 3–5 days.
- "Ayurveda or kshar sutra will cure it permanently." These modalities can help in select cases, but they have variable results for advanced grades and should be used alongside, not instead of, a proper assessment.
The Indian diet especially the Gujarati tendency toward maida-based snacks (khakhra is fine, but farsan, puri, ganthiya, and white-bread sandwiches are not) creates the perfect environment for constipation-driven piles. A small dietary shift plus one clinical visit can break the cycle.
Piles Treatment in Vadodara
Dr Samir Contractor has performed thousands of hemorrhoid procedures over 25+ years at Sterling Hospital, Race Course Road, Vadodara. Available techniques include rubber-band ligation, laser hemorrhoidectomy, stapler hemorrhoidopexy, and conventional excision — the choice depends on grade, symptoms, and patient preference.
Frequently Asked Questions
ગુજરાતી માં પૂછાતા પ્રશ્નો (Gujarati / Hinglish FAQs)
Badhaa cases ma nahi. Grade I ane II ma fibre, pani, ane cream thi ghana sudharay chhe. Grade III ane IV ma operation — laser, stapler, ke conventional — jaruri thay chhe.
20-30 minute. Sedation ma thay chhe. Saanjhe ghar jata aavo — mota bhagnu daycare ma thi thay chhe. 3-5 divas ma desk kaam shuru kari shakay.
Piles cancer nathi bantu. Pan cancer piles jevu lage chhe — etale ek vaar tari tapas karavu j jaruri chhe. 40 upar hoy ane lohi aave to colonoscopy karavo.
Roj 3 litre pani, sabji ane chhilka wali daal, whole wheat roti. Sitz bath — garma garma pani ma 10-15 minute beso. Phone lai ne toilet ma na beso. Strain na karo.
Sari rite thayela operation pachi 5-8% chance chhe ke farithi ave. Fibre ane pani chalu rakhso to chance bahu ghati jaay chhe.
Maida (puri, ganthiya, white bread), vadhu tikhu bhari na khavay. Cheese, pizza, bakery items ochha karo. Fibre vadharo — guava, papaya, palak, doodhi, turai best chhe.
Troubled by Piles?
A 10-minute OPD visit with proctoscopy tells you the exact grade and the right treatment. Most early piles need no surgery at all.